


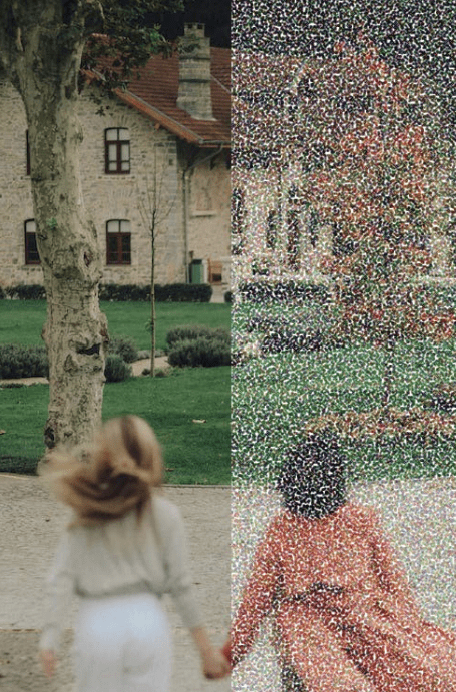
From Uncertainty to Progress and Hope
Historically, it has been challenging for people with Visual Snow Syndrome (VSS) to receive an accurate diagnosis. Due to its visual symptoms, many people with VSS and their physicians thought their eyes were the origin of the problem. But when referred to optometrists and ophthalmologists (eye doctors), who would test for abnormalities, their results typically came back “normal”. That is because VSS is a sensory processing disorder that affects vision and originates in the brain, not the eyes.
First Clinical Mention of Visual Snow
Visual snow/static was first reported in the Transactions of the American Ophthalmological Society in 1944. Frank D. Carroll published descriptions of 6 patients experiencing visual disturbances induced by digitalis, a medication for heart ailments. These included “snowy vision, flashing and flickering lights, flowerlike figures, green and yellow vision, and colored floaters”. All 6 patients underwent ophthalmic (eye) examinations, and findings were negative. Carroll surmised that digitalis impaired the central nervous system, stimulating the cerebrum to cause visual disturbances.
Today, there are various types of physicians and specialists equipped to address VSS, including neuro-ophthalmologists, neurologists, ophthalmologists, neuro-optometrists, and vision therapists who are trained in the management/treatment of VSS symptoms. But previously, VSS struggled to gain clinical acceptance.
Not Migraine, But Visual Snow Syndrome
Until recently, the legitimacy of the condition was met with doubt and marginalization. Physicians were never taught about VSS in medical school. Most of them had never heard of VSS. Among those who had, some rejected its validity.
Most assumed that VSS was simply a form of migraine/migraine aura (despite VSS patients also experiencing other debilitating visual and non-visual symptoms that were not consistent with migraine/migraine aura). The study, “Persistent Positive Visual Phenomena in Migraine” (Liu et al., 1995, Neurology), explored visual symptoms like static or snow across the entire visual field in ten migraine patients. Despite normal neurological and ophthalmological results, these symptoms persisted for months or even years. This study was critical in our future understanding of VSS.
Initially thought to be related solely to migraine aura, the symptoms described did not fully align with traditional migraines. Instead, they matched VSS, which was not recognized at the time. It was one of the first modern studies to explore the overlap and differences between VSS and migraine, ultimately helping solidify VSS as a distinct neurological condition with continuous visual disturbances, both with and without migraines.
Though some patients report the onset of VSS symptoms after a migraine, many VSS cases are independent of migraines. Unlike migraines, where visual symptoms resolve, VSS symptoms are constant, affecting individuals 24/7.
VSS: A Real & Distinct Neurological Condition
Other physicians insisted that VSS was not a “real” medical condition, falsely attributing patient reports of VSS symptoms to a psychiatric/psychological disease. This now scientifically-disproven illogical, primitive notion caused tremendous harm to the wellbeing of those with VSS and their loved ones who were seeking help. The debilitating nature of VSS symptoms coupled with the medical community’s historic marginalization, misdiagnosis, and mistreatment of VSS patients can have a profoundly negative and devastating impact on their mental health.
There were also informed physicians who knew that VSS was a legitimate, distinct neurological condition and wanted to help their patients. But without funding for further research, awareness, education, and treatment options, solutions for VSS would not be possible.
Recognition, Research, & Resources for VSS
Today, thanks to establishment of clinical criteria, global awareness, education, and research, VSS is now scientifically-recognized as a legitimate, distinct neurological disorder (with both visual and non-visual symptoms). Frequency of misdiagnosis is reducing. There is active, global research for VSS funded by the Visual Snow Initiative (VSI) that is taking place in several countries, which is revealing new information regarding the pathophysiology, biological basis, and treatment of VSS symptoms. For the first time ever, diagnostic tools, a global directory of VSS physicians, physician-patient resources, as well as noninvasive and viable treatment options are available. Moreover, following the establishment of VSI’s Diagnostic Criteria for VSS, advocacy efforts by the Visual Snow Initiative, along with VSS researchers, have clarified the relationship between VSS, migraine, and additional conditions/symptoms, reducing misdiagnosis. Helping efforts by continuing to raising awareness and supporting research are essential for improving patient outcomes globally, furthering education about VSS within the medical community, advancing our understanding of the condition, and developing solutions. Together, we can continue to make significant progress.
Please see the sections below for more information.
The Progress
VSS: At a Glance
- Visual Snow Syndrome (VSS) is a neurological disorder that can affect vision, hearing, sensory processing, and cognition; it is not a structural issue with the eyes.
- VSS symptoms affect an estimated 2-3% of the world’s population.
- Visual Snow Syndrome is named after the most common, hallmark symptom of the condition: visual snow, which is experienced by everyone with VSS.
- Visual snow can be defined as seeing static, flashing lights, and blinking dots 24/7 (with your eyes open and closed).
- Trying to see when experiencing visual snow is often likened to trying to see in the middle of a snowstorm or through a snow globe that has been shaken up, which is how it got its name.
- The first documented cases of visual snow/static vision were published in 1944 by Frank D. Carroll.
- Individuals with VSS process visual and other sensory information abnormally.
- However, VSS often entails more than visual snow, with many people experiencing additional visual and non-visual symptoms as well.
- VSS is linked to abnormal neurotransmission of serotonin and glutamate, as well and increased metabolic activity in the brain, especially visual perception and processing areas.
- VSS symptoms can be experienced from birth or at a later point in life.
- People from around the world of all ages and backgrounds are affected by VSS daily.

Challenges with Diagnosing VSS
- Optometric and ophthalmologic (eye) tests typically yield "normal" results. (VSS is unrelated to the structural integrity of the eyes; it is a brain issue.)
- Many VSS symptoms can be attributed to other conditions, causing confusion and misdiagnosis.
- VSS is often mistaken for migraine aura or HPPD, which are separate entities with different pathogenesis.
- VSS patients were often not believed, facing stigma and dismissal. This had devastating impacts on their mental health and overall wellbeing.
- It is not uncommon to see temporary visual snow, or static, especially under specific lighting conditions or while rubbing your eyes. (However, seeing these images constantly, with your eyes both open and closed, is a symptom unique to VSS.)
- Prior to the publication of scientific research, some thought VSS was a “supernatural” ability.
- Unsure what was wrong, some VSS patients were led to believe that they were going blind or their vision was deteriorating. (Researchers now know VSS does not cause blindness nor is it degenerative.)
Advancements and Milestones
- VSS is now clinically-recognized and scientifically-accepted as a distinct, legitimate neurological disorder (with both visual and non-visual symptoms) that affects vision, hearing, sensory processing, and cognition.
- VSS has been acknowledged by medical and scientific institutions/publications, such as WHO, Mayo Clinic, Cleveland Clinic, NIH, NIHR, NHS, Healthline, PubMed, Frontiers, Brain Communications, Annals of Neurology, Neurology (American Academy of Neurology), Journal of Neuro-Opthalmology, PubMed, and more.
- The rate of misdiagnosis for VSS has significantly decreased while global research for VSS has notably increased.
- New information regarding the pathophysiology, biological basis, underlying network mechanisms, and treatment of VSS has been/is being discovered.
- Through VSI, global experts are actively collaborating to study and find solutions for VSS.
- More doctors around the world have become aware and educated about VSS than ever before. They are interested specfically in helping VSS patients.
- There are now resources, educational content, and diagnostic tools to help people with VSS and their physicians.
- VSS patient care and physician-patient communication regarding VSS is becoming more effective.
- Viable and non-invasive treatment options for VSS are now available, with more potentially to come in the future as research grows.
- Thus far, the VSI team has heard from people with Visual Snow in over 93 countries affected by VSS.
- More clinical and public interest, global awareness, multimedia content, educational tools, resources, and studies for VSS are being generated than ever before.
- As we continue our work and research, additional developments are on the horizon.

Support Visual Snow Syndrome Research
All donations to the Visual Snow Initiative go directly to Visual Snow Syndrome (VSS) research.
Your tax-deductible contribution ensures that global research will continue and makes a positive difference in the lives of people affected by VSS.

