Researchers
Myrte Strik, Meaghan Clough, Emma J Solly, Rebecca Glarin, Owen B White, Scott C Kolbe, Joanne Fielding
Introduction
“Visual snow syndrome is a neurological disorder primarily characterized by visual snow, a continuous and dynamic visual disturbance across the entire visual field. A diagnosis of visual snow syndrome requires that visual snow is accompanied by at least two other visual symptoms including after images (palinopsia), light sensitivity (photophobia), night blindness (nyctalopia) and enhanced entoptic phenomena.1 Patients often experience a range of non-visual sensory symptoms such as tinnitus, depersonalization and, most frequently, migraine. In addition, patients report high levels of anxiety and depression.1,2 Visual snow syndrome onset is commonly in young adulthood3 with symptoms often severely affecting daily activities4 and independence.5 Visual snow syndrome is not uncommon, with an estimated prevalence of 2% in the United Kingdom,6 but its underlying pathophysiology is unknown and no effective treatment options are currently available.7
Although there have been relatively few neuroimaging studies conducted in patients with visual snow syndrome, altered metabolism has been revealed using fluorodeoxyglucose-PET,8,9 and altered brain activation using visual snow-like stimuli.8,10 Anatomically, grey matter (GM) volume changes have been found in relatively small areas involved in vision8,11 as well as non-typical vision regions such as the cerebellum11 and limbic, temporal and parietal regions,8 suggesting whole brain involvement, potentially explaining the wide range of symptoms reported by patients. However, the direction of volumetric change is equivocal, with both larger8,11 and smaller8 volumes reported. Whether brain microstructure is altered in visual snow syndrome, is unknown.
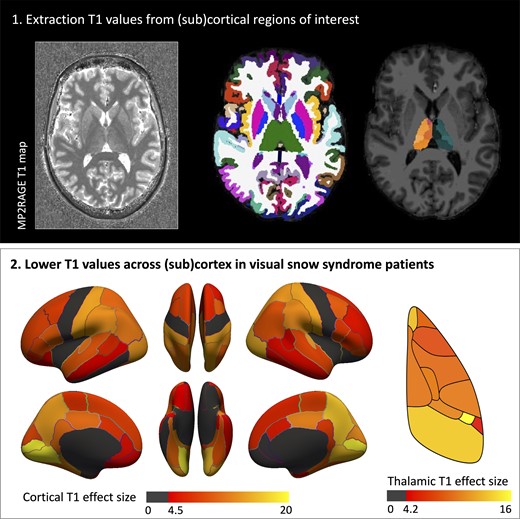
We aimed to assess alterations in brain morphology and microstructure in patients with visual snow syndrome using high resolution structural imaging acquired using ultra-high field MRI [7 Tesla (7T)]. We included patients with and without migraine to ascertain the potential impact of migraine on any changes revealed. In addition to white matter (WM) and GM volumetric analyses we assessed tissue microstructure using quantitative T1 mapping. This has not been assessed previously in visual snow syndrome. Finally, we examined whether changes in volumetrics and or T1 relaxation times were related to clinical features of visual snow syndrome and severity of psychiatric symptoms. Given the wide variety of symptoms, and changes previously revealed in visual snow syndrome, we hypothesized that these patients would exhibit volumetric changes, and potentially differences in brain microstructure.”